Oxycodone has always been a means of treating moderate-to-severe pain. Although it produces therapeutic effects and manages pain for those after surgery or people battling chronic pain, it also causes undesirable side effects. The opioid crisis, which has snowballed in severity over the years, is a cause for concern for doctors prescribing such medications.
When you go to the doctor, you’ll weigh the pros and cons to determine if oxycodone is right for you. It’ll likely mean your pain is severe enough and can’t be adequately treated by other medication or therapies. You’ll likely be referred to a pain management clinic that will have you enter into a contract to take the drug as prescribed, take drug tests to show you’re only using this medication, and follow your doctor’s advice.
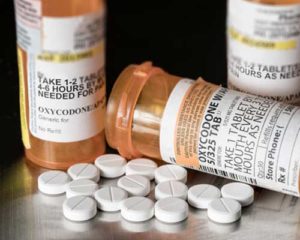 Once you’re prescribed a potent drug like oxycodone, you need to be aware of how it reacts in your body. When you start using oxycodone, it’s hard to ignore the effects it produces. You will be prescribed the lowest possible dose to relieve your pain. If it doesn’t manage the ailment, your doctor will increase the amount slightly. Over the next several weeks, the intoxicating side effects will disappear as you become more tolerant of the medication. While this isn’t always bad, it’s something you need to report back to your doctor and let them know what’s going on.
Once you’re prescribed a potent drug like oxycodone, you need to be aware of how it reacts in your body. When you start using oxycodone, it’s hard to ignore the effects it produces. You will be prescribed the lowest possible dose to relieve your pain. If it doesn’t manage the ailment, your doctor will increase the amount slightly. Over the next several weeks, the intoxicating side effects will disappear as you become more tolerant of the medication. While this isn’t always bad, it’s something you need to report back to your doctor and let them know what’s going on.
Oxycodone tolerance is the first sign of a substance use disorder (SUD). Depending on how it’s addressed, it could lead to the development of severe addiction. However, if you continue using the prescribed dose without increasing it to combat the tolerance, you’ll be OK. However, you might be wondering about oxycodone tolerance, how fast it develops, and how to manage your pain in the event this occurs.
You don’t want to become a statistic. In 2021, 75,673 people lost their lives as a direct result of their opioid addiction. While most of those deaths stemmed from the illicit opioid fentanyl, prescription drug abuse caused an uptick in these fatalities. Below, we’ll discuss how oxycodone affects your brain, how tolerance works, and how to manage your pain through other means.
How Oxycodone Affects the Brain
According to the University of California San Diego Health, about 25 percent of patients prescribed opioids like oxycodone for chronic pain will end up misusing them. Although that points to 75 percent not misusing them, it’s an unfortunate reality that chronic pain patients will suffer the consequences of those who abuse opioids. Doctors will be less inclined to prescribe oxycodone or will lower their current dose to a point where it’s ineffective.
Researchers at the university found that opioid dependence caused permanent changes in the brain. They found that oxycodone dependence causes permanent neural adaptations of the central nucleus of the amygdala (CeA) at the level of the nociceptin system. These networks are responsible for the transmission of pain. Suppressing the CeA caused GABA receptors to activate in the brains of rats addicted to opioids.
Prolonged opioid use will permanently damage the brain. We often overlook the profound effects oxycodone has on the brain, but these changes will remain even after people recover from addiction. It’s something to consider with your doctor before taking oxycodone. With an estimated 2.1 million Americans diagnosed with an opioid use disorder (OUD), seeking alternative options may be the best choice.
Oxycodone Tolerance Development
Drug tolerance can occur in as little as two weeks after use and is extremely common. It develops as a result of being regularly exposed to the medication. When you become tolerant to oxycodone, the current dose has stopped providing the desired effects. It could also indicate your body has adjusted to the presence of the drug in your system. There are a few options, including increasing the dose, changing the regimen, or considering a more potent medication. Only a licensed pain management physician can make this determination.
Oxycodone tolerance derives from genetic and behavioral elements. While it mostly occurs within the first two weeks, some people can become tolerant to oxycodone after a few times using the drug. It’s important to remember that tolerance is not the same as dependence. Even with the studies and resources to learn about it, it’s still misunderstood. One benefit researchers do see is that tolerance can lead to fewer side effects as your body adjusts to the drug.
What Are the Effects of Oxycodone Tolerance?
Those becoming tolerant of oxycodone may be at a crossroads. Tolerance is the first sign you’re developing an opioid use disorder, meaning it’s time to make a decision. If you’re in severe chronic pain, your doctor will consider prescribing you a higher dose or using more potent opioids to combat the problem. However, if you’re not experiencing relief from oxycodone and want to take more because of how it feels, it might be time to consider stopping.
The effects of oxycodone tolerance indicate the current dose is no longer working. You may be inclined to start taking more, but this will surely lead to you becoming dependent on the drug, meaning you’ll experience withdrawal symptoms if you lower the dose. When you become dependent, you’re only taking oxycodone to avoid withdrawal symptoms and not experiencing its effects. If you continue taking the medication at higher doses, you’re in dangerous territory – this is when addiction can occur.
Can You Reverse Oxycodone Tolerance?
Fortunately, oxycodone tolerance can be reversed. It may not be easy, but it’ll benefit you in the long term. Some of the most common treatment options to lower your oxycodone tolerance include switching to longer-acting opioids, slowly tapering your dose, or treating the symptoms of opioid withdrawal. Tapering your dose is the most common means of reducing your tolerance. It consists of gradually decreasing the amount of oxycodone you take over time. The process allows your body to adjust to the lower dose and reduces the severity of cravings. It’ll also help your body with pain relief since lower amounts will be more effective.
How to Manage Pain Without Oxycodone
Whether you’re battling chronic or acute pain, it can have a devastating toll on your mental health and life. This is a cruel reality for many people, and using opioids might be their final line of defense. Effective pain management allows for improved function, giving individuals peace of mind and their lives back. However, to find effective treatments that don’t consist of narcotics, you must speak to your doctor for nonopioid options.
A conversation with your doctor will determine the course of action. They’ll ask you questions to learn about the following:
- How pain is impacting your life
- What you’re looking to gain by managing your pain
- Your health history
These detailed discussions will teach your physician about the goals you have, in turn allowing them to identify the best treatment that poses the lowest risk level. To manage the pain, you must know the different types.
For example, acute pain typically appears suddenly with a known cause, such as surgery or injury. It typically subsides as the body heals. However, chronic pain, which is pain that lasts three months or more, can be caused by an injury, disease or condition, inflammation, or something unknown.
There are various non-narcotic options available to manage your pain. Some work better than others, but all have fewer risks and side effects than oxycodone. Depending on the type of pain and its severity, doctors will consider the following:
- Topical ointments, such as lidocaine
- Acetaminophen (Tylenol) or ibuprofen (Advil)
- Exercise therapies, such as physical therapy
- Exercise
- Weight loss
- Interventional therapies, such as injections
- Depression medication
- Seizure medication
- Cognitive behavioral therapy (CBT), which helps a person learn how to alter their responses to pain and stress
- Acupuncture and massage
Some or a combination of these options will lead to your pain management goals. You must work with your doctor to make a plan. When crafting one, remember the following:
- Be open to pain management without opioids.
- Understand that pain relief doesn’t happen overnight.
- Talk to your doctor about which options could result in success, and contact a specialist if needed.
- Follow up with your doctor regularly and provide them with progress reports.
- Know your options.
